This article first appeared in Enterprise, The Edge Malaysia Weekly on August 5, 2019 - August 11, 2019
In 1997, the government launched the Telemedicine Blueprint — a move that was driven by a vision that one day, patients would no longer need to travel to see their doctors. They could just video call or chat with them
But the idea may have been a little ahead of its time. The internet was not as well developed nor were technologies such as the Internet of Things (IoT) and artificial intelligence (AI) commonplace at the time.
“Back then, Skype was just being introduced. It was so grainy that I gave up after a while,” says Dr Wong Chee Piau, professor of paediatrics at Perdana University and founding member of the Telemedicine Development Group.
But technology has evolved and the ideas that were mooted more than two decades ago are still relevant.
“They had fantastic ideas and we are still talking about these now. One was the idea of establishing a personal lifetime health record. Their ideas were ahead of their time, and the technology was not able to keep up,” says Dr Wong.
Nowadays, telemedicine is only a small part of the larger realm of digital healthcare. Patients can monitor their heart rate and blood glucose levels with wearables, such as a patch or watch, while their doctors can monitor for abnormalities remotely. Patients can also contact their doctors via video call and get their prescriptions mailed to them. The latter (e-prescription) is already available at Putrajaya Hospital.
Perhaps the biggest sign that digital healthcare is becoming a huge trend was when Ping An Good Doctor — China’s biggest online healthcare platform — formed a joint venture with Grab last August to expand into Southeast Asia. It has an AI-assisted chatbot that refers patients to appropriate doctors. It has also piloted unstaffed clinic booths in China that provide online consultations and basic prescriptions.
In Malaysia, a group of doctors and entrepreneurs are looking to further that vision. In 2015, they began organising an annual telemedicine conference. In 2017, they set up the Telemedicine Development Group. Last year, they changed the name to Digital Health Malaysia (DHM) to better reflect the scope of their work.
“It encompasses everything from data management to healthcare delivery and how the ecosystem enhances the service. Now, we have more people who are aware of it and the technology is more capable. We just have to keep evolving with the challenges,” says Dr Wong.
Some of the members of DHM are doctors turned entrepreneurs who designed solutions based on their own pain points. For example, Dr Prathaban Raju, co-chairperson of the DHM’s Special Interest Group 1 (SIG), is founder of Door2Door Doctor. The others have different backgrounds, such as former consultant Hazwan Najib, who is founder of DoctorOnCall Malaysia.
There are four SIGs under DHM to look at regulations, knowledge dissemination, R&D, certifications and go-to-market strategies. Ministry of Health (MoH) director-general Datuk Dr Noor Hisham Abdullah has provided crucial support for their work.
DHM is eager to promote a regulatory environment that welcomes start-ups to the sector. It also wants to create an ecosystem with health practitioners, regulators, entrepreneurs and technology providers.
“Digitalisation is inevitable. Patients will constantly look for options [that can be delivered] on their devices. That means some non-qualified person can start selling their services,” says Dr Prathaban.
“If consumers can chat with a robot in the Czech Republic tomorrow, they will. Will they end up seeing a doctor online in the Philippines? What if the patient has a wound infection? How will that doctor understand the local hospital system? Will we then get Lazada to ship medical equipment in bulk [to the consumers]? That is dangerous.”
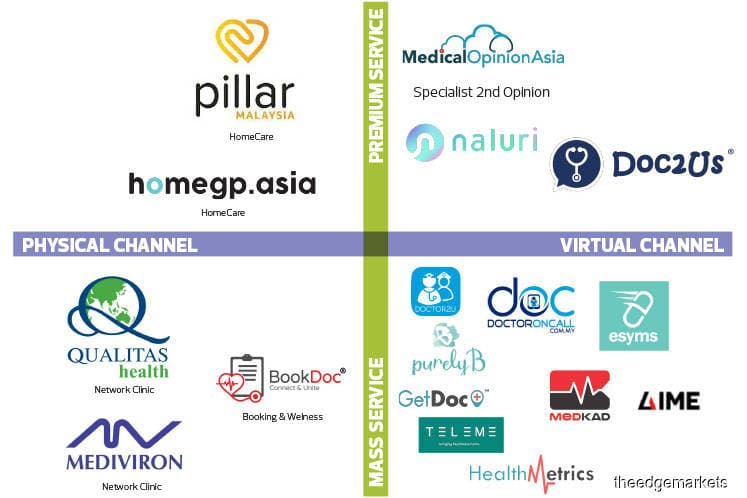
There will also need to be some kind of balance struck between online and offline care, where patients get advice and prescriptions from certified healthcare providers online and still get in-person care. That is why there must be communication between the various healthcare players, says Dr Raymond Choy, co-founder and CEO of Doc2Us, an online consultation platform that allows patients to chat with doctors via text messaging.
“Going entirely online will not work. But if you do everything in bricks-and-mortar form, you will not be relevant anymore. So, how can we adopt technology and still merge the service with that of healthcare providers?” says Dr Choy, who is part of DHM. He used to be a general practitioner and emergency responder for the Raffles Medical Group at Changi International Airport in Singapore.
If Malaysia does not jump on the bandwagon, the local digital health entrepreneurs will leave the country due to difficulties in getting past regulators and raising funds, says Dr Prathaban. “I was lucky that I bootstrapped and managed to survive, although I still faced a lot of trouble with my start-up.
“A lot of companies cannot even get through the six-month runway. What happens when they are waiting for approvals from the various agencies? Or when they are waiting for lawyers to talk to the insurers but the lawyers do not really understand the laws you are governed by?”
Technology will improve the provision of care for patients and reduce costs as clinics do not necessarily have to be staffed 24 hours a day, he adds. You could have a call centre with teams that specialise in providing different types of services.
“Healthcare is not a need that goes away. My aspiration is to get regulations and policies streamlined and give start-up founders a chance to be leaders in the digital healthcare space. Malaysia has the potential for that,” says Dr Prathaban.
A matter of regulation
Much like how Bank Negara Malaysia has a regulatory sandbox for financial technology start-ups, DHM wants to set up one for digital health start-ups with the MoH and the Malaysian Communications and Multimedia Commission. The two government agencies are also part of DHM.
Under this arrangement, start-ups can provide their services in a safe environment and suggest which regulations are outdated. “We could have the sandbox and SIGs bring together all the stakeholders — regulators, grassroots players like myself and hospitals. We need to come together and figure out how we can digitise healthcare because it is the least disrupted industry,” says Dr Choy.
This sandbox will be important because complying with regulations is one of the biggest challenges faced by start-ups. According to Dr Prathaban, Malaysia has more than 25 laws governing healthcare. These need to be updated to catch up with innovation. Also, regulators should look at the laws on healthcare data, data privacy and medical devices, among others.
“How can we emulate the best practices in healthcare in the virtual space? For instance, how can electronic medical records comply with the Personal Data Protection Act? How will data residency laws change how we share information? All these guidelines and protocols are very important for patient safety, especially as we are moving from being paper-based to digital. We have to be very careful,” says Dr Prathaban.
Some countries are already doing this. Australia is implementing regulatory reforms for the medical applications of 3D printing while the US Food and Drug Administration is monitoring digital health products such as medical mobile apps and medical software. According to reports, the MoH is planning to implement an electronic medical record system in 145 hospitals nationwide over the next three years, thus facilitating the sharing of patient information.
Other areas that require change include training for healthcare providers, who may not be comfortable with technology. The industry also has to future-proof its software and services according to international standards, says Dr Prathaban.
More investors and funds needed for digital health
Another issue is the difficulty in securing funding. This is a complex industry and it is difficult to find investors who really understand it.
“If they do understand, it is from a consumer perspective or they have a superficial knowledge of the healthcare industry. Very often, a non-healthcare investor may just believe in the team or use metrics that do not apply in this space. They may also not appreciate how much value healthcare start-ups bring to the ecosystem,” says Dr Prathaban.
This is in contrast to hospital operators that have money to invest, he adds. “Yet, they often struggle to implement the right solutions effectively in a traditional healthcare business model. I believe we have good start-ups in Malaysia that have innovative solutions. So, how can we bridge this investment gap?”
Meanwhile, Dr Choy observes that it is difficult to get seed funding. “The venture capital and private equity firms tend to fund later-stage start-ups because they have proven models,” he says.
On top of everything else, the funding space is fragmented. Dr Wong points out that Malaysia has many funding agencies, but these are not properly targeted. The government should address this issue and ensure that the research in local universities can be translated into products.
“Innovations need to go through a few phases, each of which requires funding. First, funding is needed to turn an idea into a prototype. Once this has been done successfully, the prototype needs to be tested. Then come the clinical trials. Finally, funding is needed to turn it into a workable product and have it commercialised,” says Dr Wong.
The difficulty is in getting funders to figure out which stage they should be funding. Ultimately, DHM’s goal is to bring together stakeholders, set up a sandbox and provide suggestions to regulators.
“Collaboration is key. We are an inclusive organisation and we hope that anyone who is interested in this industry will collaborate with us,” says Dr Wong.
The start-up story
Many digital health start-ups have emerged in Malaysia in the last few years. One of them is Door2Door Doctor, founded by Dr Prathaban Raju in 2013 after he had to take care of his father.
“In 2012, my father was diagnosed with liver cancer. That led me to start the company and offer all the services that a home care patient would need, such as doctors, nurses, physiotherapists, blood tests, caregivers and transport. I was taking care of my dad and realised that a lot of people need these services,” says Dr Prathaban, who was a general physician at a primary care clinic.
He sold the company in 2017. The platform provided on-demand and subscription-based services for home care. It supplemented the service of caregiving with technology, both at the front and back end. “My passion is in combining medical care with technology,” he says.
After he sold his start-up, he joined Strateq Health Inc, which builds back-end IT systems for hospitals. “We do this for 23 hospitals. Now, I provide consultancy to companies that are in or are looking to go into healthcare technology,” says Dr Prathaban.
Similarly, Dr Raymond Choy, founder of online consultation platform Doc2Us, began his journey after his father was diagnosed with leukaemia. He was then practising medicine at the Raffles Medical Group in Singapore.
“I had to keep sourcing for doctors, haematologists and oncologists. We were very blessed to have a network to connect my father to good doctors. But it was quite a complicated case and he died after three months,” he says.
Dr Choy then thought about those who did not have easy access to doctors. “I think my colleagues, like myself, have had this experience where our family members and friends text or call us to ask about their medical conditions. All this led to the idea of creating a platform so that everyone could have simple access to a healthcare provider.”
He and his co-founder Jack Lee set up Doc2Us in 2015. But they found that Malaysians were unfamiliar with paying for online consultation services. “We felt like we were a few steps ahead of the general population. So, we pivoted and began to serve pharmacy partners, clinics and corporate clients. We also have e-pharmacies and e-labs solutions,” says Dr Choy.
Individuals can still use its free online chat service to talk with newly graduated doctors, who are carefully selected, tightly monitored and supervised by the company’s medical board. These new doctors are restricted from prescribing medication.
In June, Doc2Us became the first in Malaysia to launch a Digital Signature-powered e-prescribing solution that fully complies with the Digital Signature Act 1997. The start-up connects prescribers (doctors) to community pharmacists, who are the dispensers within the controlled enclosed ecosystem.
“A lot of times, we know our [doctors’] handwriting can be challenging for pharmacists to comprehend, which may contribute to errors. We also wanted to digitise this and make every record well-kept so they cannot be tampered or changed,” says Dr Choy.
“Electronic prescription is good but not secure and safe enough. So, we need an authorised third party to identify the prescriber and dispenser. That is where the digital signature comes in to enhance the authorisation and security processes. We are doing this for the safety of patients by providing a digital platform for doctors to communicate with pharmacists in a safe and secure environment.”
Working to create the future of healthcare
Dr Wong Chee Piau, professor of paediatrics and a founding member of Digital Health Malaysia, is an expert in paediatric neurology. Much like the other doctors, he has ideas to improve the healthcare service. One is to create an Uber-like platform for healthcare, where patients can go to an open marketplace to look for services.
Second, he envisions a central database for small and medium enterprises (SMEs) in the digital healthcare space. “When you talk about digital health, it is not just about a device. You need to maintain a database and you have to analyse the data. We propose a platform that SMEs can use to store data and make use of the analytics platform. That will lower the cost of entry,” says Dr Wong.
He wants to turn that into a virtual hospital, where if a test needs to be done, for example, the patient can just go to the nearest laboratory. The results will be sent electronically to the doctor. Once the results are out, the patient can get the medicine from the nearest pharmacy, which has already received the e-prescription.
He also has ideas for dealing with epilepsy, which is his area of interest. “I have an app where parents can press a button and put a timestamp on when the child has a seizure. They can record it and show the doctor. That is linked to the child’s personal health record, so we know when the medication is given and its impact on the seizures,” says Dr Wong.
He is also trying to create a wearable that can detect epilepsy. A lot of parents spend sleepless nights worrying that their child will go into seizure. This wearable and app will be able to monitor the child at night.
Dr Wong is also incorporating epilepsy genetics and pharmacogenetics into the platform to better understand the complex relationship between epilepsy and genetics.
CREST
Collaborative Research in Engineering, Science and Technology (CREST) is looking at healthcare as a sector prime for technological disruption. It has already assisted three innovators to conduct clinical trials of their high-tech solutions in Malaysia, in collaboration with the Ministry of Health and industry partners.
This thrust began in 2014, when CREST began to look at how the Internet of Things (IoT) and artificial intelligence (AI) could be used in the healthcare sector. “The idea was to use AI and other technologies to help people stay healthy rather than reacting only when they fall sick. That was what drove us to bring our community into the healthcare industry,” says CEO Jaffri Ibrahim.
CREST was set up in 2012 by leading E&E players, local universities and the government to drive R&D and innovation in Malaysia. It is the place where researchers go to make their ideas come true. After all, leading E&E companies such as Advanced Micro Devices, Intel and Keysight Technologies are among its founding members.
“We (Malaysia) have about 40 years of history in that (E&E) sector and we have seen people from the community innovate. For example, there was a guy whose father had diabetes and almost died. He then quit his job at a multinational corporation and developed a wearable device. When the patient sweats at night, the wearable will check the sweat content to see if the blood sugar level is too high. It will then inform the family to check on the patient,” says Jaffri.
The person went on to start a company and tried to sell his products. Unfortunately, the company did not make it. “But that is the nature of business in the devices and E&E sector,” says Jaffri.
CREST will facilitate innovation by helping to turn ideas into products and connect the inventors with the right people, be it regulators, investors or Digital Health Malaysia. It also provides funding at the idea stage.
“We do not have funding yet for the full cycle that I think is required for this industry. But we are trying to convince the government that there is a gap in funding and we can help fill it. That way, the innovation can go all the way and become a proud Malaysian solution that we can offer to the world,” says Jaffri.
Stethee, an AI-powered stethoscope, is one example that he mentions. It was not invented by Malaysian scientists, but the founders wanted to manufacture that product here. The medical device is approved by the US Food and Drug Administration and is currently undergoing clinical trials by the Ministry of Health’s family medicine specialists and others.
“We are also about to embark on a project where we use the Stethee to record the normal heart sounds of the nation. Once we have that, we will open up our database and ask scientists to study abnormal heart sounds that indicate asthma, for instance. We will have the capability to develop algorithms that can detect abnormalities in people and treat these at an early stage,” says Jaffri.
Another initiative under R&D and commercialisation is the Malaysia Retinal Reading Centre (MyRRC). Diabetic eye disease is the most common cause of loss of vision among adults of working age in the country. Through this project, AI algorithms will be developed to diagnose diabetic retinopathy in various stages. MyRRC aspires to be the national reading centre that can screen and grade thousands of retinal images per day from public and private healthcare facilities.
Yet another initiative is an AI-assisted bone fracture detection system, which is under trial at two hospitals in the Klang Valley.
Save by subscribing to us for your print and/or digital copy.
P/S: The Edge is also available on Apple's App Store and Android's Google Play.
